Research led by UCLA Fielding’s Dr. Olivia Jung recognized with “2025 Best Theory to Practice Award” by Academy of Management
Research led by UCLA Fielding’s Dr. Olivia Jung has been recognized with the “2025 Best Theory to Practice Award” by the Academy of Management.
Research led by a UCLA Fielding professor has been recognized as among the best in the field in 2025 by the leading professional association for management and organization scholars.
UCLA Fielding’s Dr. Olivia Jung, assistant professor in the Department of Health Policy and Management, is a scholar of organizational behavior, general management, and health policy. Peer-reviewed research she co-led was recognized this month by the U.S.-based Academy of Management (AOM) as the “Best Health Care Management Theory to Practice Award” for 2025.
“It is truly an honor for our team to have been recognized for our work,” said Jung, who has worked on similar questions about organizations as disparate as community health centers and NASA. “We are at a juncture where health care practitioners are facing incredible pressure, diminishing resources, and increasing expectations for success. My hope is that our work advances conversation around how experts can interact with and support teams working day in and day out to improve how we care for our community.”
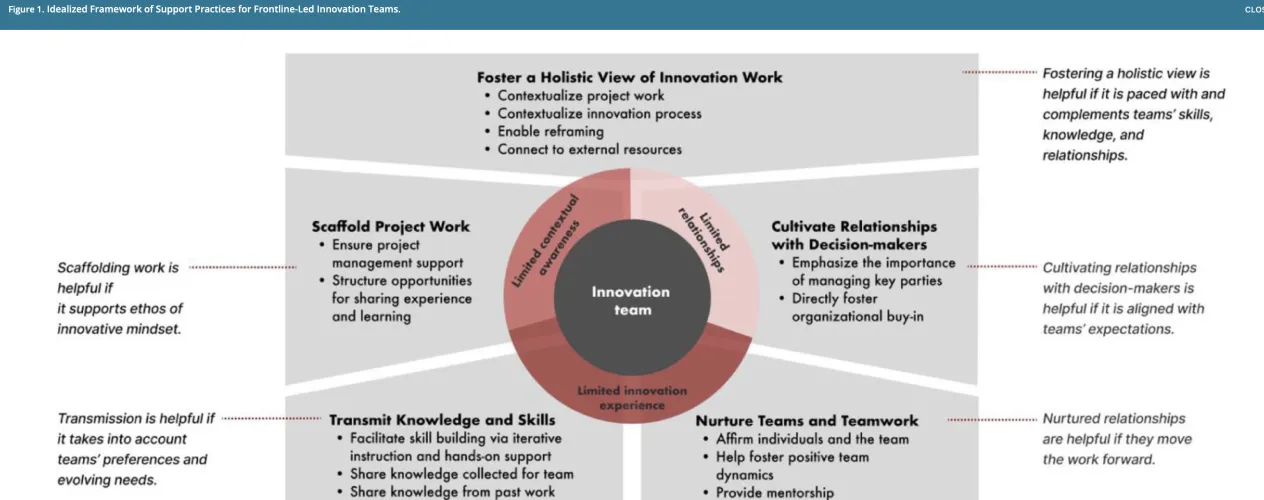
The peer-reviewed study – “The Dynamic and Multisource Nature of Support for Frontline-Led Innovation Teams” - was published in November in the journal Medical Care Research and Review; Jung’s co-authors included researchers with New York University, Columbia, and Stanford. The team conducted a 24-month study of six frontline-led innovation teams at federally qualified health centers, and their research produced three core findings.
First, effective support must be adaptive: the most helpful supporters shifted their approach based on each team’s specific barriers, whether limited innovation experience, weak organizational relationships, or gaps in contextual awareness. Second, a “net of support” outperforms any single expert—teams benefited most when technical and relational support worked in concert across multiple roles. Third, some of the most impactful contributors were unexpected: student fellows, a managed care insurer, and a private funder all emerged as critical sources of support, often because their loosely defined roles gave them the flexibility to fill gaps that formal coaches could not.
The findings have direct implications for healthcare organizations of any size, Jung said.
"Even without a structured innovation program or resource support, recognizing the value of distinct support roles -contextualizing policy, building organizational buy-in, scaffolding project management - can meaningfully improve how frontline teams are equipped," she said. "We also caution that poorly structured support can backfire: innovation programs that pile onto staff workloads risk exacerbating the very burnout they aim to address."
The AOM award, sponsored by the academy's Health Care Management division, is intended to encourage papers relevant to practicing health care managers by clearly addressing research questions relevant to the translation of theory to health administration or management practice, officials said.
“When we think about how teams work together, their challenges, and their successes, we generally focus on direct team members,” said co-author Dr. Patricia Satterstrom, an assistant professor of public service with NYU’s Robert F. Wagner Graduate School of Public Service. “But a team’s success is dependent on more than just their members. It is influenced by the circumstances they operate within and the external support they receive. That is where our paper shines a light: On the people – the supporters – who can influence a team’s success and the types of support that are most beneficial.”

